|
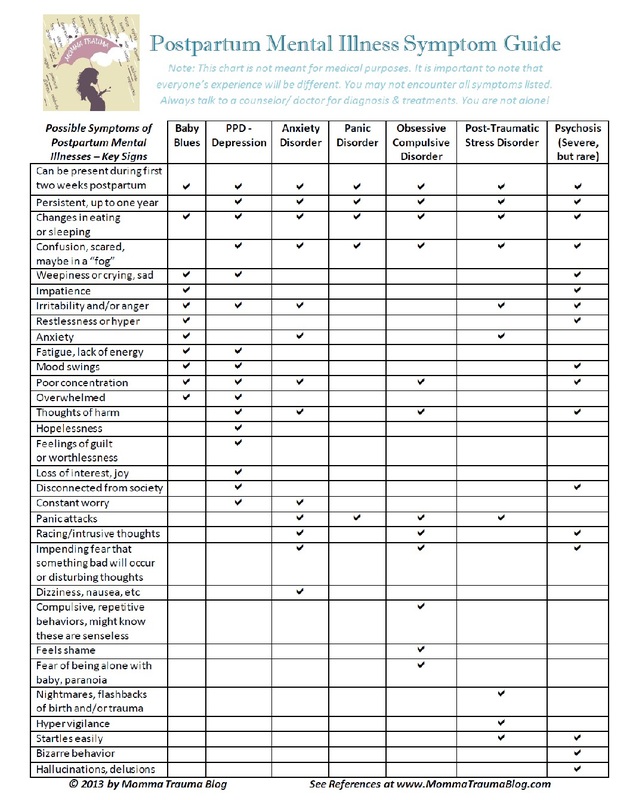
This is a post for our More than Baby Blues series. Pin this story to Pinterest! Up to 80% of all moms have symptoms of Baby Blues during the first weeks after childbirth. With all our hormones going crazy, it's no wonder! Baby Blues is most often categorized by short-term random crying, anxiety and fatigue to name a few symptoms. Its symptoms often overlap with other postpartum mental illnesses, so how do we know what is *really* going on in our own heads? There are a few key signs to look out for in the first few weeks to determine if you or your loved one might have Baby Blues or something more. Lasting no more than two weeks, Baby Blues is just that: The "blues." A parent dealing with Baby Blues will still be able to enjoy their new baby and think clearly (as much as the lack of sleep will allow with a newborn). A parent wanders into the territory of "something more" when symptoms persist longer than two weeks or sooner if they creep into the functioning of every day life activities. Serious symptoms such as thoughts of harm and hallucinations should be addressed immediately. It's imperative that you are honest with yourself and your loved ones about thoughts you might be having so you can get the needed help as soon as possible. I am a give-it-to-me-straight kinda girl and I realized there were no side-by-side charts to differentiate disorders from one another, especially Baby Blues. Sure, you could search and search online like I did to get a somewhat decent glimpse of all six disorders and Baby Blues. But hopefully, this guide is a little easier to understand. Please remember that you should always seek the advice of a counselor and/or doctor in regards to diagnosis and treatment. It is normal to not have every symptom in a disorder. It is also normal to have more than one at once. If you suspect you might be suffering from more than Baby Blues, go talk to a professional. You are not alone. You are normal! As my mom always says: "It's the crazy ones who don't seek help!" If you would like a copy of the PDF file for this chart (better quality, great for clients and local families!), comment below or e-mail me and I'll send it to you. What do you think? Let me know your thoughts in the comments below! References:
FOLLOW THE SERIES:
10 Comments
 Jenni from Mindful Serenity shared her story with Momma Trauma. Check out her blog for great discussions on faith, sustainable living, pregnancy losses, pregnancy, parenting and more. I'm so grateful for her opening a part of her to us as she shares her story with Postpartum Anxiety and losses. "Regular readers will know that I had been through several miscarriages prior to my first live birth. I experienced a lot of depression during and after those, and credited it to grief, although I knew that there could be chemical components to it too. When I did realize I was going to carry to term with this one, I was shocked to find that I was still depressed. I was depressed for most of my pregnancy, in spite of being extremely excited that I was finally going to have a baby. I anticipated that I might have postpartum depression, and tried to have a support network in place just in case. I have a family background of depression, bipolar, anxiety attacks, and even severe panic-induced breakdowns. But aside from the depression I mentioned here, I had never experienced any of those things myself. I'd never had an anxiety attack let alone chronic anxiety. When my baby was born, I was jubilant. Our circumstances were actually really bad, my husband was working two jobs because we were broke, and it was the middle of winter. But I was not depressed. I was delighted to have a baby. But I was terrified of hurting him. I have eight younger siblings and had been helping with babies for two decades before I had my own baby. I knew how to handle diapers and baths and feedings and all those things, and yet I still found myself feeling scared all the time. I was afraid that he would stop breathing in his sleep. I was afraid that as I laid him on the bed that his arm would twist under him and break as I set him down. When I had him in the sling as I made dinner, I was afraid that he would reach out and touch a pan or get cut on a knife or something before I could prevent it. I was terrified that he would get badly hurt and that it would be my fault. Not an accidental kind of fault, but a totally preventable kind of fault. None of these were rational fears, but they all ran around in my head on a daily basis. I never told anyone. I assumed that I was paranoid about this baby because of the years of miscarriages and the waiting for him. Of course I was hyper-protective of this baby! And I could tell that they were irrational fears, so I didn't tell anyone because I felt stupid for having them. By the time he was about 6 months old they went away. Three years later I had a second baby. I had not had difficulty conceiving or carrying him. The delivery had been straightforward and good. But I had experienced pregnancy depression again, and I had the postpartum fears again. This time I couldn't justify it to myself, because I didn't have the same set of circumstances coming in. I had HAD a baby before and everything had been fine with him. I couldn't think of why I would feel paranoid this time around, but I did. And it was the same things...stopping breathing, breaking his arm...knives in the kitchen... Sometimes real things did happen. Like when he was 3 months old but had gotten strong enough that he kicked so hard that he tipped his bouncer over. He had been on the floor and was scared but not hurt. I was not much distressed by this, I comforted him, and just accepted that he had gotten too big for the bouncer and didn't use it anymore. But I was still scared that I would hurt him somehow. Again, when he was a few months old it faded. That baby was two when I listened to a podcast where a woman talked about having had postpartum anxiety. I had never even heard of such a thing. Her case had been so serious that she was institutionalized for several weeks (away from her baby). I was grateful that my anxiety was not that severe, but I also felt so validated in my experiences. I wished I had told someone. I wished I had known what it was. Now that I know (and it's only been a year that I've known) I have started telling people. Nobody should have to deal with this kind alone. It's scary and unnerving and it would have been nice to know that I wasn't crazy." Thank you Jennie, for sharing. Your courage to speak out will help a parent who might not know where to turn. View her original post here. Jenni co-founded the Amethyst Network, which seeks to offer miscarriage support and advocacy, especially in the form of networking doulas to attend miscarrying women. If you would like more information on donating, volunteering or networking, check out their site or Facebook page. Do you have a personal experience to share on birth trauma or postpartum mental illness? It's comforting to see that others have been in your shoes before, at least a little bit. Comment or e-mail your stories. Anonymity is always welcomed if needed.  Image courtesy of marin/freedigitalphotos.net Image courtesy of marin/freedigitalphotos.net How often do you think you resemble an undead creature who moves very slowly and is not really with it enough to be aware of the things going on around you? Everyday for you, too, huh? It seems to be an unwritten, daily requirement in mommy territory. Zombie Prep Dad, as my husband has recently named himself, would even venture to tell you Zombie-ness affects dads far too often, too. But do you think your inner Zombie attacks more frequently than it should? Brainnssss…. Toddlersss….. Coffeeeee….. (speaking of which, I need to make another pot, but I digress!). There’s definitely a level of Zombie that most parents deal with on (usually) a daily basis. Especially when you have the young children still running around, laundry to do, dishes to hand wash, dogs to let loose outside so they don’t let loose inside, a partner to feed and keep mildly happy at least, meetings to attend or run, possibly a business or work to contend with, volunteering, church, keeping in touch with friends, the lists really could go on and on. And all this on little to no sleep. But hey, as long as we have a coffee pot running all day, we’re good, right? What happens when that’s not enough? Depression, PTSD, Anxiety, OCD and other postpartum mental health disorders can turn the every-day, lack of sleep Zombie (or Mombie as some call us!) into a different Zombie altogether. We may not even realize what is happening to us at first. We might say, “No, it can’t be. I’m not crazy! It’s just Baby Blues and I’ll snap out of it soon.” You may be happy one second, and angry or sad the next. It’s certainly different for everyone. Depending on the illness of course, this Zombie can often be affected by a murky fog that keeps reality at a distance. I’ve been in that fog, and it’s no Zombie picnic. For me, it was a fog from post-traumatic stress disorder and depression. I eventually found myself trudging through life, clinging to the clock in anticipation of everyone leaving for the day to go to work so I could break down again. Some days I wouldn’t even be able to wait that long and I would just cry no matter who was home, not able to hide the tears. But when asked what was wrong, I would simply mutter, “I’m just so happy to be with my baby” because I didn’t want them to know the truth and think I was crazy. I didn’t even believe the truth myself. What was the truth? Truth was, I didn’t want to nurse my baby, or hear her cry, or hear her coo. I definitely didn’t want to deal with our 16 month old toddler who was into everything. I adored naptimes, because when I wasn’t crying, all I wanted to do was sleep and who can’t sleep with an infant on your chest? Otherwise, I didn’t want to be touched. Sex was pretty much out of the picture because of the depression AND ptsd, I definitely wasn’t taking care of myself like I should. But, at least the kids were dressed and fed, right? I would wonder why I was there. I would tell myself, if it weren’t for the kids needing their mother around, I might not stick around. (I’ve gotten past that, I promise) I tell you all that because postpartum mental illnesses, not baby blues, can be as dangerous as deadly. It’s okay to feel down, anxious, stressed, overwhelmed… What’s not okay is not seeking help. “Help” is different for everyone. I encourage anyone who struggles with mental illnesses at any point to see a counselor, someone who is qualified to diagnose and counsel you through this patch in life. Seeing a counselor doesn’t automatically mean you have to go on medications, it just means you need someone to help sort out your thoughts a bit. When I meet with friends, birth doula clients or well, let’s face it, I try to talk to every pregnant mom I can because I could just talk boobs, placenta’s and uteri all day long… I always emphasize the importance of knowing which key signs of postpartum mental illnesses to look for, especially to the partners and loved ones I meet. It is so important to understand that no matter how well educated you are on the topic, you may not realize that YOU might be going through something more than just Baby Blues. Because of that, it is imperative (especially for those of us with a history of mental illness) that those closest to us understand the signs of postpartum mental illness in the event we don’t see it ourselves. Over the next week, we will set our Zombie, coffee-filled sights on each postpartum mental illness (and Baby Blues!) and discuss the warning signs we and our loved ones can keep in mind. I’ll try to keep it light and easy to ready, because if you wanted to read a textbook on mental illness, you’d have gotten one already I’m sure! If you have dealt with a postpartum mental illness and wouldn’t mind sharing your story, or even a glimpse, please comment below or e-mail. Anonymous is always welcomed. Do you want this series delivered straight to your inbox? Subscribe to Momma Trauma! To repin this story on Pinterest, click the image above or here. STAY TUNED: Friday, A dad-blogger will talk with us about Postpartum Depression in Dads! Stay tuned for more posts throughout the week. FOLLOW THE SERIES: 
NOTE: This post is from a momma in our Facebook community. Image courtesy of David Castillo Dominic/FreeDigitalPhotos.net
By Eli Leblanc, member of Césarimouski There are three types of women in our society. Those who shave (or wax or whatever) their legs, those who don’t, and those who shave but wished they had the guts not to. I’m in the last category. I’m not proud of it, but yes, I crack under social pressure and I don’t show my legs in public passed a certain length of hair. Each summer, I make a point of stretching my limits at least once, hoping that one day, I will be strong enough not to care. But truth being told, I don’t like having hairy legs. I don’t find it sexy at all. For some people, this is perfectly normal. We don’t shave for others, we do it for ourselves, right? Well I see things differently. Adults naturally grow hair on their legs. Finding it ugly on women is not coded in our genetics. We let society teach us that hair is disgraceful on women’s legs. Well I should be stronger than that. My mom once told me that she hoped one day I would accept the fact that I shave my legs. I immediately snapped back “Why don’t you wish me to accept my hairy legs instead?” In the end, it leaves us with 2 choices. Accept our weakness, or try to get stronger. Personally, I aspire to get stronger. The same concept can be applied to my birth trauma. Accepting my weakness would be letting society tell me that it was not my fault, that I did the best I could, that I am not to blame. Who knows, maybe if I said those words often enough I would actually end up believing them. But I choose to try to get stronger. I want to take my responsibilities and admit my share of blame. I don’t want to “shave” my faults away, I want to leave them intact and, eventually, learn to accept them. The birth of my children couldn’t have been less empowering. Maybe this could be? Ahah! I know what you are thinking! That accepting your weakness also requires a lot of strength. Yes, I have thought about that one, but stick to my point: one day, I hope I will find the courage to show my hairy legs! Momma Trauma's Thoughts on Hairy Legs By Momma Trauma I can see a lot of validity in Eli's words and thoughts here. As a birth worker and activist, I often tell moms: Be sure that whatever decision is made for you or your baby, it is made by you after informing yourself on the topic. It's so important to OWN our decisions, not just in birth, even if it means accepting and taking the responsibility for our own faults. When I birthed our first born, we had quite the typical medicalized birth. Going to the hospital as soon as my waters broke led to pitocin which led to pain medication (I'm lucky the epidural guy was late and I couldn't get that!), which led to more pitocin and more pain medication, which led to shoulder dystocia which led to a broken collar bone in my son. I'm grateful and blessed it did not end in a c-section. I quickly learned that not only was I not broken as the doctor stated and that everything could have been prevented, I learned that I could have been the one to prevent it all. Everyone said, Oh it's not your fault, momma. He just got stuck, he was a big baby after all (if you consider 7.5-ish lbs big). When, in reality, I made the choice to not invest in a good childbirth education class and instead took a two or three hour overview on childbirth taught by nursing students who were only concerned with a class grade. I also made the choice to not do my research, ask for clarification, blindly follow the doctors, not hire a doula, the list goes on. *I* bear sole responsibility for what happened in those wee hours in labor. That was a tough lesson to learn, but as soon as I did that, it was like a weight had been lifted off my shoulders. And I made damn sure to do my research for baby two. Sure, I could have agreed with the multitudes of people telling me it wasn't my fault that his collar bone was broken. But it didn't sit right. Weakness would have been remaining complacent to societies whim and letting that dictate how I felt and how I would birth future babies. Strength was learning to say No, that's not right and moving forward to better myself and my babies' futures. Whichever route you take, make it your own. Eli and I happen to have very similar stories in terms of weakness and strength. Other women may tell you their own weakness IS their strength. Some may tell you their strength is their weakness. Which are you? Do you shave? Do you let your legs be what they are naturally? Or do you shave and wish you didn't? Do you have a story to share about embracing your weakness or strength? Everyone's journey is different! Comment below or e-mail your story. Guest posts are uploaded every Friday, the next one could be yours!
Yesterday I went to my new OB/GYN's office for appointment one of two to get my IUD removed. I went alone because after rescheduling a few times, it was too late for anyone else to rearrange their schedules. I guess I hadn't thought about this appointment for a few days because about half way there I remembered it was with a male doctor.
*Enter Trigger* I talked myself down. I was driving. That was no place to have a panic attack about the inevitable exam that would occur shortly. Luckily, a friend had called to keep me 'company' on the ride. I pull in 15 minutes before I had to walk inside and start filling out 'new patient paperwork' (which ended up just being quick HIPPA forms). I sat in my van crying. Trying to pull myself together enough so the receptionists wouldn't think I had hormone issues. Momma Eli was online and keeping me company all the way from Quebec. I pull myself together again and slowly wander inside after 10 minutes of anxiety over seeing the doctor. Inside, the reception was kind. She handed me the forms and went on about her business. I started to freak out a little more. The office smelled just like the hospital I delivered in. The floors looked just like the hospital floors. I thought perhaps they have to go by a standard flooring, like standard procedures, like my 'standard procedure.' I really couldn't get over the smell. It made me nauseous. Eli reminded me to sing a song I could think of without too much thought. I think I surprised her when I first thought of Celine Dion's early French songs. (LOVE Celine!) She also suggested I write down a brief note to the doctor so I didn't have to explain why I was so upset and have that note act as my 'partner.' All I could write was this: "Hi. I'm Jenn. I have post traumatic stress disorder from giving birth to my daughter 23 months ago." That's all. Maybe next time I should just print out this entire blog instead. I tried not to cry in the waiting room, but tears came anyway. And I was shaking. Not enough to be noticeable though I don't think. It didn't take long to be called back to an intake room where a nurse took my weight and height. I've lost 6 pounds. Way to go me! I thought to myself, "I should tell this nurse what's up. I'm sure she can alert the doctor before he has to ask me." But I couldn't muster even that. I'm not sure why, the words just wouldn't come out of my mouth. And of course, I wished I had written more in my blurb suggested by Eli. She asked intake questions such as do you smoke, do you drink, how many times have you been pregnant, how many live births.... This only made the tears come faster. But I didn't want her to see me crying. I just couldn't tell her. How would she understand? She left the room and I reached for a tissue. And I grabbed my notebook to write down what I was feeling so I could come back here and tell you all about everything. Again with the smell. And the floors. And now it sounded like everyone was stomping around in the hallway. Do sounds heighten when you're panicking or anxious? She came back in to escort me to a patient room and noticed I had been crying by now. She asked if I was okay, I nodded. Why couldn't I tell her? So now, I wait. With the smell, and the floors, and the really loud stomping people in the hallway. There's laughing in the hallway, have you ever noticed nurses and doctors do an awful lot of laughing while patients are impatiently awaiting them in rooms? They were awfully loud. I stared at the bed that is in every patient room with the examining lamp next to it and could see myself getting an exam. I could see myself getting THE exam from when our daughter was born. When I was violated, it was a hospital bed, but of course this bed signifies the same exam that is about to happen. Shaking again, I heard a male in the hallway. I felt like throwing up. I didn't. I shook more with each door creek, until my own patient door creeked open. I quickly finished writing notes in my notepad which was on my lap. I thought to myself in a split second: I have to pee. I downed my coffee right before I walked in. That was stupid. The doctor barged into the room like a bull in a china shop. He joked about the essay I must be writing in the notebook and nearly snatched it off my lap. "Just some thoughts," I mumbled. I felt like a child right then. He sat in his chair and hunched down to eye level with me. Then he started talking to me like a two year old. I felt disrespected. He talked to me like I didn't know anything about my body or birth control. He was also very loud. But maybe that was hypersensitivity. I shook some more as he talked AT me. He finished his one sided conversation about my IUD and told me to "take (my) bottoms off so (he) could explore what was going on." I'm not sure why, but that made me really cry. I was done. I blurted out the question asking if he'd have a nurse in the room with him for the exam. I knew the answer would be yes. I'm not sure why I felt the need to ask, but I did. The answer was indeed: yes, of course. Followed promptly by: "Oh. You're crying. Why are you crying? Did you want a female doctor? Why didn't you get a female doctor?" Me, blubbering: "They had scheduling problems." He continued to freak out a little bit and rushed me to the receptionists to reschedule with a female doctor. And he rushed off. I'm sure he was freaked. I'm sure his reaction was standard. I'm sure he didn't want to put me through something I didn't want to go through, and I greatly appreciate that. Maybe I'll write him a note. I do wish, though, that he would have taken a few minutes to decompress with me and let me answer why I was crying. I would have answered. And I would have been okay. I think. But, he's an OB/GYN, not a therapist. I get it. I was both relieved and disappointed. I guess I'll have to try again in March with a female doctor. I thought I was okay afterwards, but I was so agitated all day. My husband took the day off from work to be with me and our kids, even though I told him to go. I'm glad he didn't.  Nationally recognized Certified Professional Midwife Karen Webster has been under fire by Delaware officials claiming she "practiced medicine without a license," and thus gave her a cease & desist order. Upwards of 50 or more supporters attended her hearing in Dover, De on Jan. 17, 2013 including children, mothers, fathers, grandparents, birth professionals, a doctor and others where Webster presented her case for midwifery versus medicine with just herself and an advocate as she could find no lawyer to take her case. The State of Delaware still seems displeased with her actions and defense. She wrote the following update on her Save The Midwife facebook page last night: "I am sad, but not surprised to say that I got the answer to my Delaware hearing and it was 28 pages - not in my favor. So the hunt for an attorney with the cojones to fight this fight with and for me begins again in earnest. I fight this for all the midwives who have or may be charged with "practicing medicine without a license" when what we practice is NOT medicine, but midwifery...I need your help, those of you in DE who believe that you should have access to qualified, licensed midwives for your homebirths." What can we do to help? Sign our petition: to change regulations to allow Certified Professional Midwives (CPMs) to obtain permits to practice in Delaware so that families have the right to choose how they give birth. Licensure of CPMs will support an integrated maternity care system. Attend the upcoming Delaware Birth Network meeting: Wed. Feb. 20 at 6 p.m. at the Kent County Public Library in Dover, De. Join the Delaware Friends of Midwives, the consumer group that is specifically for CPM licensure. Donations: "In a world where it feels like everyone is always asking for money, where we sometimes find ourselves wondering where the money we spent has actually gone, please be assured 100% of your donations will go DIRECTLY to Karen Webster, CPM. Click here to donate through Paypal. Click the "transfer" tab then "send someone money". From there enter our email [email protected] and the amount. You don’t have to have a Paypal account and you can use your credit or debit card. Karen’s dedication to the natural process of birth has changed countless lives, let us join together and donate to changing hers." - From the Save the Midwife Website Write to Delaware state legislators and other influential persons, including Governor Jack Markell: Karen asks us to "write to Governor Jack Markell about his Executive Order # 36, which called for a review of all DE statutes and regs that DE citizens thought were NOT working and ask him to review the testimony given at those meetings held this past October in Kent and New Castle counties, in favor of changing the regs to allow CPMs to get permitted to practice and stop being prosecuted!" FOLLOW THE STORY:
What will you do to help? What are your thoughts on Karen Webster's case or the midwife crisis in the United States?  NOTE: This post is from a momma in our Facebook community. By Eli Leblanc, member of Césarimouski I never made the decision to breastfeed my children. I didn’t need to. Female mammals carry their babies to term in their wombs, they push them out when time comes, they breastfeed. I’m a female mammal and I never questioned those obvious mammal behaviours. The birth of my first daughter was a really traumatic one. I was expecting an empowering natural birth at the birth center; I ended up having a c-section under general anesthesia without my consent. It took hours before I finally met her and even then, I was still stoned. C-section, drugs, mother-child separation, trauma. The conditions were far from ideal to initiate breastfeeding. But I did. And for the first few days I thought we were doing well. By day 5 however, there was still no sign of lactation. She was still losing weight. We had given her water because dehydration was causing fever. I eventually agreed to start supplementing her using a supplementing nursing system (SNS), thinking, or hoping, that it was only temporary. Despite all my efforts to stimulate production (frequent nursing, pumping, medicinal supplements, drugs), I never had sufficient lactation. Mixed feeding was for me a big disappointment. I kept thinking “carry to term – CHECK, push out – FAIL, breastfeed – FAIL. 1 out of 3, well done...”. Of course, I felt like a failure for not being able to breastfeed exclusively. And not because “society” put too much pressure on me. When it comes to pressure and guilt, I am quite self-sufficient, thank you very much! In the end, it turned out not to be a complete disaster however. Thanks to the SNS, I only introduced the bottle when she was 8 months, because I was going back to work and seeing me coming for lunch to nurse her at day care seemed to trouble her more than anything else. I thought that it would be simpler to switch for the bottle at home as well, keeping the breast for comfort. By then, her attachment for the breast was secure enough, the proof being she is now 4 and I am proud to say that I still nurse her everyday! My breastfeeding issues are definitely a part of my trauma, first as a consequence, then as a cause, since I now associate my whole birthing experience including post-natal to my trauma. But I am convinced that breastfeeding saved me from post-partum depression. After what I went through, not being able to breastfeed at all would have been the last blow. “Breastfeeding is much more than feeding”. That obvious but important statement from my midwife and the fact that she got me a SNS were life savers. It is while nursing my baby that I felt the first sparkle of attachment when she was 3 weeks old. It was subtle and timid, but she made a cute little face as she was suckling and I interpreted it as content. For the first time, I felt that I was really her mother, that she was happy to be in MY arms and taking MY breast. When she was 15 months, I got pregnant. I knew a lot of kids were weaning themselves during pregnancy. I was hesitant about tandem nursing at first, thinking that I had not managed to nurse one properly, but I also thought it would be a good way to stimulate my production if needed. So I opted to let her decide what would happen. She nursed throughout my pregnancy. She was used to not having much milk from there anyway. I was really hoping that giving birth this time would ensure a proper lactation. I prepared physically and psychologically for a VBAC, but in vain. My second daughter was also born by c-section. Although that one was not as traumatic (at least I was conscious!), I was still devastated, even more considering that I had by then decided that this child would be the last one. My hopes to repair what was broken by having a good birthing experience were gone. Breastfeeding was my last battle. After 24 hours, and despite all my efforts trying to reassure myself, I was already starting to stress about lactation. An acquaintance (she eventually became one of my best friends!) visited me at the hospital. I was surprised at first. We didn’t know each other well, but we both had difficult birth experiences and shared the same convictions about breastfeeding. We talked a little and when she saw how worried I was about not having a proper lactation, she spontaneously and generously offered to pump some milk for me, just in case I had to supplement my daughter whiles waiting for lactation. I accepted her offer with a lot of gratitude and she manually extracted about 1 oz in my room. I immediately felt better, knowing that if it came to that, at least I wouldn’t have to give junk food to my little one. Indeed, 2 days later, my daughter was showing signs of hypoglycaemia and jaundice and I still had no sign of lactation. Even the few drops of colostrums I was able to extract at the end of my pregnancy were gone. I did not have the energy to fight the medical team, so I accepted to start supplementing using the precious milk in a SNS. I thought I would have to fill 15 forms in 18 copies to have the “right” to give real milk, but they impressed me for once by simply accepting my choice. From that time, my new friend and I agreed that she would give me all the milk she could for the first few weeks and that we would reassess the situation depending on my lactation. When it turned out to be insufficient, again despite all my efforts including having a toddler to stimulate my production several times a day, she decided to boost her production, using medicinal supplements. By the time my daughter was 5 months, she was still providing more than half the supplements I needed. It meant that on some days, my baby was exclusively fed breast milk! She was even following the weight curve of an exclusively breastfed baby! I couldn’t have cared less if I had actually been breastfeeding exclusively, but under the circumstances, it was a small victory. When we saw each other, it was simpler for my friend to nurse my baby directly. Some of my other friends also decided to donate some milk sporadically, or to nurse her directly. This co-breastfeeding experience had a real positive outcome on my moral. Although I still had some problems accepting that I did not produce enough milk, I had the satisfaction of giving the best second choice. My daughters are now 4 and 2, and yes, they both still take the breast. The youngest weaned herself from the SNS when she was 16 months. I still haven’t accepted their birth. As for breastfeeding, it has for me a bitter-sweet, but rather sweeter, taste. Of course it still hurts that I relied on mixed-feeding rather than breastfeeding exclusively. Is it only related to the traumatic birth or do I also have a physiological problem limiting my ability to produce milk, I will never know. But breastfeeding definitely helped me bond with my children. Tandem nursing brought me a rewarding feeling I never thought was possible considering the situation. As for the co-breastfeeding, that was a pure act of generosity, love and support from my friends and as a traumatized momma, I sure needed plenty of that! For another glimpse in Eli's healing story, read When what did not happen hurts even more than what did. Much love to you, Eli, from Momma Trauma! Your story strengthens me, and you always inspire me to think deeper! Have you had permanent struggles relating to your birth trauma? Happy Valentine's Day everyone! Take some time to love yourself. Love, flowers, wine, brownies, all that good stuff. (Don't mind the face for radio! Videos make me nervous, lol.)
Coercive-Violence, or coercive-force, is the idea that someone uses the threat of harm, or harm itself, to compel someone else to a desired end result. It happens in every type of relationship, or between strangers. It can be a complicated concept, so I hope to break it down enough to easily understand in this post.
As a human right, we should be able to give our go-ahead (or lack thereof) to things which will happen to our bodies. That freely given, clear go-ahead agreement is called Consent. When we don't give our consent, or are unable to do so, the action in question would then become non-consensual if it were to still happen. Pretty simple, right? Here's an example of lack of consent: I told him No. What is NOT considered consent?
Then we move on to the term: Force. When we think of force, images of physical altercations usually come to mind such as holding someone down or physically pushing them to do something. But there's an emotional aspect to force that many do not consider. Merriam-Webster defines force as:
Now we need to bring the term Coercion into play. Coercion is when someone uses fearful or forceful statements, words or acts to compel the person to make a certain decision or action. It is also described as extreme peer pressure, threatening, manipulation, badgering and/or bribing. Here's an example of coercion: I was told my child(ren) would be harmed if I did not agree. Putting it altogether, we can see that a non-consensual decision can sometimes lead to Coercive-Force or Coercive-Violence. If we feed together the examples listed above, we get this statement: "I told him no. He held or tied me to the bed. I was told my child(ren) would be harmed if I did not agree." I could think of a few scenarios off the top of my head to go with that statement, including birth stories, and none of them are okay. In no circumstances should it be okay to use coercive-violence. Even in childbirth. (Did that just spin your head around? Let me say it again...) It's is not okay for a birth worker or medical professional to:
For more on violence during childbirth, check out this post or What is Perinatal Violence. Momma fan Carolyn McAfee, of CCMcAfee Photography in Western NY, sent in this beautiful and healing dance called Calling All Angels for our Blog Carnival against violence against women in honor of One Billion Rising's global V-Day event. Read the words, listen and watch closely to the movements which depict (at least to me) a woman in need of healing, support and above all, doesn't want to go at it alone.
Special Note: Carolyn is the main dancer! Song: Calling All Angels By: Jane Siberry Oh, a man is placed upon the steps, a baby cries High above, you can hear the church bells start to ring And as the heaviness, oh the heaviness, the body settles in Somewhere you could hear, a mother sing Then it's one foot then the other as you step out on the road Step out on the road, how much weight, how much weight? Then it's how long and how far and how many times Oh, before it's too late? Calling all Angels, calling all Angels Walk me through this one, don't leave me alone Calling all Angels, calling all Angels We're trying, we're hoping, but we're not sure how Oh, and every day you gaze upon the sunset With such love and intensity Why, it's ah, it's almost as if you could only crack the code You'd finally understand what this all means Oh, but if you could, do you think you would Trade it all, all the pain and suffering? Oh, but then you would've missed the beauty of The light upon this earth and the sweetness of the leaving Calling all Angels, calling all Angels Walk me through this one, don't leave me alone Calling all Angels, calling all Angels We're trying, we're hoping, but we're not sure why Calling all Angels, calling all Angels Calling all Angels, calling all Angels Walk me through this one, walk me through this one Don't leave me alone Calling all Angels, calling all Angels We're trying, we're hoping, we're hurting, we're loving We're crying, we're calling 'Cause we're not sure how this goes Thanks for the beautiful dance and thought, Carolyn! If you have a chance, please check out her blog and wonderful photos! And her Facebook page! |
AuthorWelcome to Momma Trauma's Blog! Thoughts, empowering posts and stories straight from Momma Trauma herself, Birth Trauma families & birth professionals. Archives
July 2015
Visit our Sponsors
This space is available for text advertisements. See our Sponsorship page for more information! xxxxx
|

 RSS Feed
RSS Feed


